In Ghana, a country of 26 million people, there are only about 20 ear, nose and throat, or ENT, physicians practicing at any one time. Limited access to ENT care in the West African country has led to high rates of chronic ear conditions that, when left untreated, can cause permanent hearing loss and life-threatening illness.
The University of Michigan Department of Otolaryngology-Head and Neck Surgery has been collaborating with physicians in Ghana to develop more robust ENT education and facilities there — particularly for otology, or diseases of the ear. The department recently established a medical education partnership with the ENT residency program at Komfo Anokye Teaching Hospital, or KATH, in Kumasi.
U-M faculty began visiting KATH in 2015, initially to assess patient needs and supply the hospital with medical equipment for otology care and training. During each trip, the team leads ENT courses and surgery simulations for KATH attendings and residents, and tends to its patients in the clinic and operating room.
Michigan photographer Roger Hart accompanied the department on one of their first trips to KATH, capturing the early stages of a collaboration committed to impacting long-term change.

U-M's ENT partnership with KATH is modeled after OB-GYN training programs U-M helped establish in Ghana 30 years ago. Timothy R.B. Johnson, M.D. (Residency 1979), professor and chair of U-M's Department of Obstetrics and Gynecology, forged that original partnership, and saw potential for similar success at KATH. "Our training partnerships have developed leaders who have gone on to be important change agents improving care in Ghana," he says.

Greg Basura, M.D. (Fellowship 2012), assistant professor of otolaryngology-head and neck surgery and leader of the partnership's otology specialty, says the medical education partnership has emphasized training KATH's two main ENT attendings, Rita Larsen-Reindorf, M.D., and Issahalq Duah Mohammed, M.D. "The impetus is on them to train the next generation of physicians," he says.
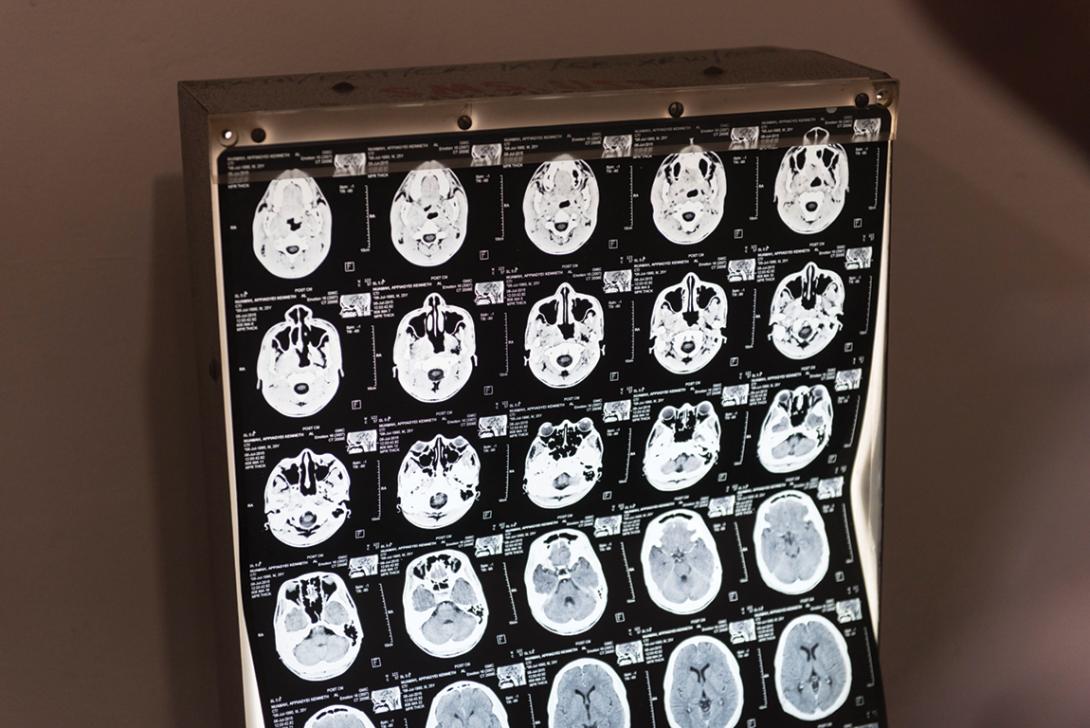
Larsen-Reindorf and Duah attend lectures about skull-based anatomy, ear anatomy and pathology, and learn how to screen patients for ear drum perforations and chronic infection. The curriculum is designed to prepare them for KATH's most pressing otology needs: caring for severe middle ear infections and cholesteatoma — a bone-eroding skin growth in the middle ear.

The department has traveled to KATH a total of four times, with another trip planned for March 2017. Basura says the two attendings are showing great skill and are beginning to better understand operating room processes. "They're improving on their diagnoses, and their scope of practice is expanding."
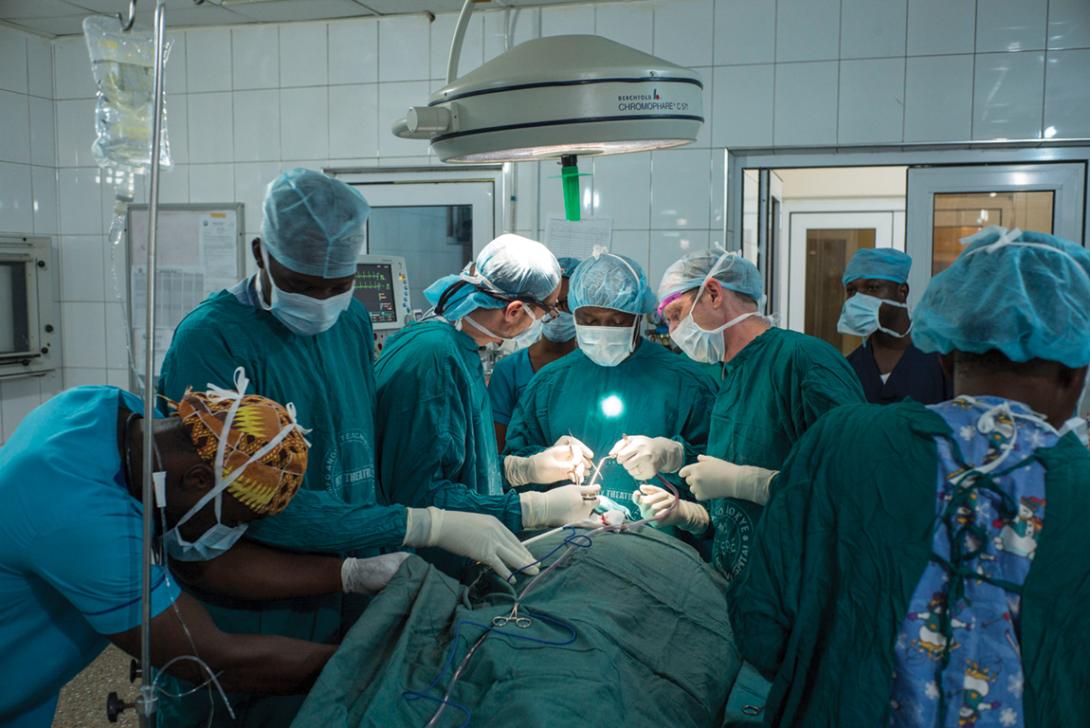
Basura, Mark Prince, M.D., interim chair of otolaryngology-head and neck surgery, and Jeff Moyer, M.D. (Residency 2003), associate professor of otolaryngology-head and neck surgery, set up a temporal bone simulation lab to train ENT specialists how to drill through bone at the cranial base during ear surgery. Basura, who gave the first ever temporal bone drilling course in Ghana, knows this type of lab is essential.
"This is a long-term medical educational partnership," he says. "We're helping them build the foundation for epidemiological research. If I can look back on this in 30 years and say 'Wow, look at what they're doing. This training is interwoven into their residency. These docs can better manage the disease and serve the people of their country,' that's really what it's all about."





