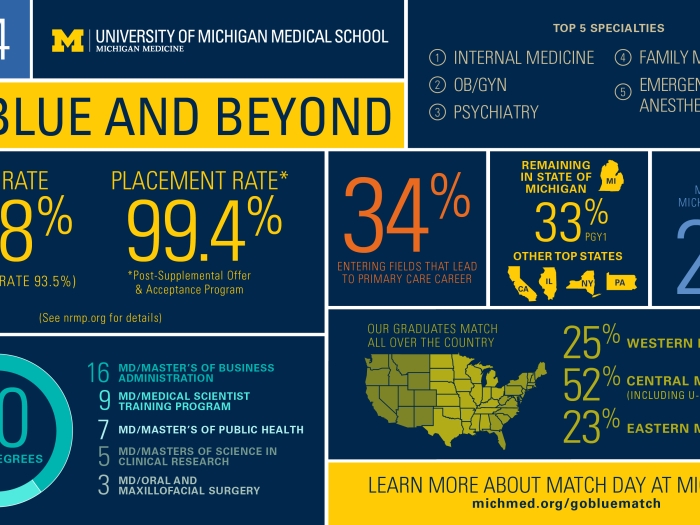
The Paths of Excellence program allows medical students to explore everything from new inventions to ancient methods of healing.
Author |

A deep dive into knowledge that a traditional medical school curriculum would not cover. A social-scientific community with peer-to-peer networking and professional collaboration. A "capstone" project that could lead to a life's work. Having professional impact while still a student. And regular engagement with a faculty adviser. These are the opportunities that made U-M Medical School students first take interest in and ultimately flock to supplemental programs of study called Paths of Excellence.
Early in this decade, aware that peer institutions were revamping curricula to address individual and societal needs, a group of U-M Medical School deans, associate deans, and other administrators proposed to address those needs with a new, optional curricular track. Many topics presented themselves, but the group settled on Global Health and Disparities (GHD), which would allow students, through study and final capstone projects, to become agents of sustainable change, reducing domestic and global health disparities. Leading with GHD allowed the school to make a moral statement about global responsibility and responses to societal needs. Twenty-five students signed up. With its small-group student immersion gatherings, one-on-one advising, and capstone projects, GHD was also positioned to be a template for more of what would become the Paths of Excellence. GHD began in 2013 under the direction of Brent Williams, M.D., MPH, associate professor of internal medicine and a member of the Institute for Healthcare Policy & Innovation. Given the success of GHD, the Medical School administration began thinking what other tracks it might offer.
"It really took a village," says Heather Wagenschutz, M.A., MBA, today a co-director of the Paths of Excellence, describing the process that followed. The Medical School administration called together a large group of students, faculty, staff, and deans whose mission was to formalize and create more paths. They tapped Wagenschutz and Eric Skye, M.D., associate professor of family medicine, to lead a workgroup to create more paths and to co-direct the overall program. (Skye has since been succeeded as co-director by Catherine Kim, M.D., MPH, associate professor of medicine, of obstetrics and gynecology, and of epidemiology.)
During the first few years of development, the GHD helped shape the Medical Ethics and Health Policy paths. Then, using a data-driven, student survey approach coupled with input from the workgroup, Innovation and Entrepreneurship, Medical Humanities, and Scientific Discovery were added in 2014–2015. The two most recent paths — the Scholarship of Learning and Teaching, and Patient Safety, Quality Improvement, and Complex Systems — began in 2016.
"Every single path is unique," says Wagenschutz. "Some are more regimented; some are more open." The goal is to introduce students to scholarly material that augments traditional classroom learning and enriches their medical training, often by introducing unusual points of view.
"We want students to go beyond the typical research paper or abstract," says Kim. "We want them to own the project." So far, students within the program have produced research projects, a nonprofit, a book of poetry, medical devices, and a set of public health guidelines. The program operates on a lean budget but is sustained in part by some 70 faculty advisers and mentors. Some of the eight path directors — administrators who assemble the core path teams and run the paths in cooperation with Kim and Wagenschutz — also advise. Although most advisers have medical degrees and training, a capstone might instead require an adviser with a background in law, philosophy, the arts, or another field. "All the advisers and directors," says Wagenschutz, "bring their own unique talents and expertise to the table and help move the mission forward."
Student response to the Paths of Excellence has been strong. Even though a Path of Excellence is not required to graduate, in 2017–2018, 75 percent of students followed one. And the future looks even brighter. Out of some 175 first-year medical students, 160, or about 91 percent, have expressed an interest in following a path.
Medicine at Michigan recently interviewed six students, all pursuing different Paths.

GLOBAL HEALTH AND DISPARITIES
MIGUEL ROVIRA (M.D. 2018): "Facilitators and Barriers to Raising Children in High-Risk Families in Low-Income Neighborhoods in São Paulo," a qualitative study
PATH DIRECTOR: Brent Williams, M.D., professor of internal medicine
Rovira grew up speaking both English and Spanish at home, and he studied Portuguese and German in college. He chose to attend U-M not only for its curriculum, but because he could continue and expand his study of global health, thanks to the Medical School's Global REACH program, which has helped the Global Health and Disparities Path expand rapidly. Faculty and students have developed partnerships with sister institutions abroad, working on everything from improving patient care to working with NGOs or governments on developing health policy — "a universe unto itself," as Rovira says.
Prior to enrolling, Rovira approached Michele Heisler, M.D., MPA, associate director of Global REACH, about her research in Brazil. Heisler had followed a cohort of Brazilian children born in 2012, and, in order to determine mortality factors, assessed the children at regular intervals. For his capstone project, Rovira worked on semi-structured interviews (pre-determined open questions combined with opportunities for the interviewer to explore certain themes or responses further as they see fit) to similarly evaluate health outcomes in poorer Brazilian neighborhoods.
"Michele had tested semi-structured interviews to assess health outcomes with families in Detroit," he says. "We wanted to implement these interviews with a similar demographic in Brazil, and we wanted to evaluate the personal, individual approach to health care taken by community health workers going house-to-house in Brazil."
MEDICAL ETHICS
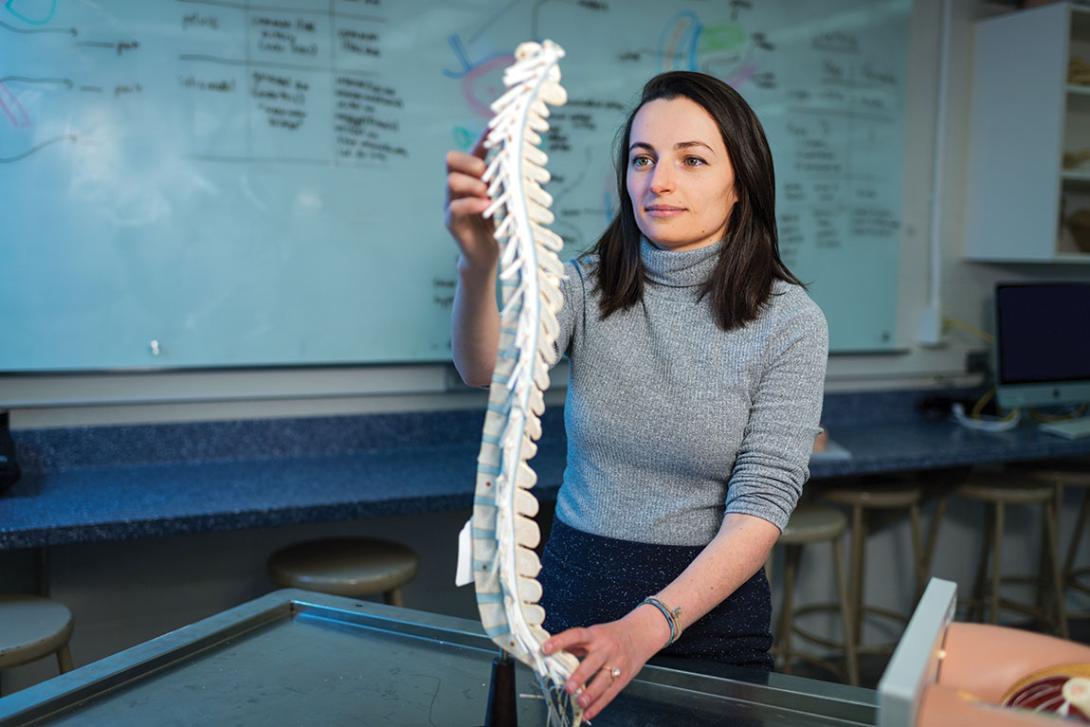
MEGAN LANE (M.D. 2018): "The Ethics of Anatomical Donation: A Body of Work," a published article
PATH DIRECTOR: Lauren B. Smith (M.D. 2002, Residency and Fellowship 2007), director of hematopathology
Lane came to the Medical School with a double major in biochemistry and women, gender and sexuality studies, and she read widely outside the sciences. She wanted to incorporate humanistic thought into her medical education. "Joining a Path let me interact with a small group of students with a common interest," she says. Lane chose the Medical Ethics Path. "In the hospital I got to do ethics consults in real time," she explains. For her capstone, she chose the history and ethics of anatomical donation, which caught her interest during her first-year anatomy lab.
Lane gives an unsettling history of how medical schools have obtained cadavers. "The bodies of institutionalized individuals were used in the 19th century. Then there's a period in which it becomes unclear how they got the cadavers," she says, alluding to the practice of grave-robbing. "Until about 1950, medical schools still had relationships with state institutions, and then transitioned to donation programs seen today." Her mentor on this project was Christian Vercler, M.D. (Fellowship 2013), assistant professor of plastic surgery. In 2016, Lane presented at the American Society for Bioethics and Humanities conference and published an article in the AMA Journal of Ethics about these issues. She is guest-editing an issue of the AMA Journal of Ethics this year in her chosen field, plastic surgery. "Megan will leave medical school with a unique body of work that she owns. She can build a career out of this," Smith says.
Today, Lane is examining the ethical questions behind commercial products like Alloderm, a biomaterial used in plastic surgery made from the skin of donated cadavers, and considering areas such as the regulation of aesthetic.

INNOVATION AND ENTREPRENEURSHIP
TAYLOR NOVICE (third-year medical student): Hot Spot Smart Socks for Patients with Diabetes, product development
PATH DIRECTOR: Mark S. Cohen, M.D., associate professor of surgery and pharmacology
"I wanted to differentiate my medical school experience," says Novice. "I wanted to gain a background in medical technology, because tech is integrating so much into medicine."
During the summer of 2016, after Novice's first year of medical school, Cohen helped her get a summer internship at IncWell, a venture capital firm in Birmingham, Michigan, where she screened and sourced medical device companies and learned how to take a product to market.
Following her summer internship, Novice enrolled in FFMI fastPACE, an accelerated biomedical innovation and commercialization course offered by Fast Forward Medical Innovation at U-M. The Paths of Excellence in Innovation and Entrepreneurship often partners with FFMI to provide programming and learning opportunities to promote medical innovation. Using her FFMI fastPACE experience, she joined a team of fellow students participating in the first U-M Medical School "Shark Tank," based on the reality TV show in which would-be entrepreneurs present to investors. "We identified clinical problems," Novice explains, "then pitched solutions to a panel of M.D.s."
Novice's team already had spoken with Chandu Vemuri (M.D. 2004, Residency 2011), an assistant professor of vascular surgery and one of the "sharks," who described the problem of diabetic neuropathy leading to foot ulcers, which, in turn, frequently lead to lower-leg amputation. Checking one's feet visually is insufficient because, by the time visible inflammation forms, it can be too late. What if diabetic patients could identify potential areas of foot inflammation early on?
Working with six U-M engineering students, Novice's team came up with Hot Spot Smart Socks. The friction that can cause ulcers produces heat, detected by the socks' thermochromic material. The color of the sock then changes, alerting the patient to the inflammation. The socks became the capstone project for Novice and her teammates, and they are in the process of applying for a patent. With 1.5 million diabetics worldwide susceptible to foot ulcers, the health benefit could be significant. And Taylor and her colleagues are looking to expand. The use of thermochromic materials to measure friction and pressure has many other health applications, including wheelchair coverings to help paraplegics avoid pressure ulcers and diapers for patients with dementia.
"Taylor has learned to evaluate medical challenges," Cohen says, "design solutions, and move her idea toward commercialization and patient impact. These skills will help her throughout her career as a physician-innovator."
SCIENTIFIC DISCOVERY
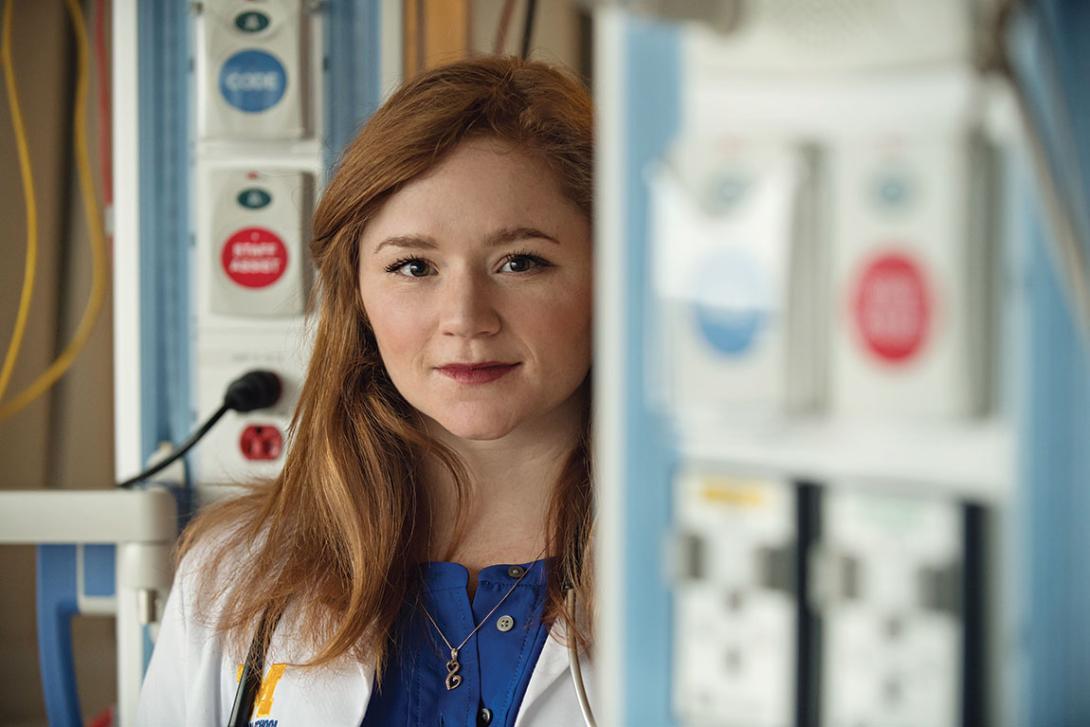
KATIE GILBERT (third-year medical student): "Elevated White Blood Cell Counts Correlated with Outcomes in Infants Undergoing Cardiac Surgery," a research paper
PATH DIRECTOR: Benjamin Margolis, M.D., professor of internal medicine
"I thought about an M.D./Ph.D., but a Path of Excellence was a great way to develop research skills without adding years to my education," says Gilbert. "My interest in research comes from my engineering background. I studied biomedical engineering at Johns Hopkins University, with a concentration on cell and tissue engineering. I always want to understand how things work and how to make them better. Research encourages creative thinking. What questions can you come up with? How can you answer them to improve patient care and patient outcomes?"
Margolis had introduced Gilbert to John Charpie, M.D., Ph.D. (Fellowship 1995), professor of pediatric cardiology at C. S. Mott Children's Hospital. The Michigan Congenital Heart Outcomes Research and Discovery program (MCHORD) also lent support. "We all believe that our students must lead in research," Margolis says. "We try to engage them in research, show them what a research career looks like, and equip them to compete for NIH dollars."
Charpie became Gilbert's research mentor and suggested that a correlation between pre-operative white blood cell counts — biomarkers of systemic inflammation, measured by the patient's neutrophil-to-lymphocyte ratio — and cardiac surgery outcomes in infants was a worthy research focus. Research showed that, in adults, elevated white blood cell counts correlated with poor outcomes for those undergoing cardiac surgery, but the issue had been overlooked in infants.
"We found that an elevated pre-operative white blood cell count means an infant will probably not do well post-surgery," Gilbert says. "Now, we must find a special marker for the outcome. The ultimate goal would be an intervention — for example, administering a steroid — that would lower the white blood cell count and thus improve the outcome for the infant." As Margolis puts it, "All research tries to help patients as much as we can and deliver care in the most effective ways." Moving toward that goal, Gilbert's the team will now seek IRB approval for further research into how neutrophil-to-lymphocyte ratios correlate with outcomes.

HEALTH POLICY
REGINA ROYAN (M.D. 2018): "Self-Regulation in the Age of Urban Revitalization: Evaluating Lead Dust Fallout from Residential Demolitions in Detroit, Michigan," a research paper that resulted in best practices for demolition that are now in place in Detroit
PATH DIRECTOR: Susan Goold (M.D. 1987), professor of internal medicine, and of health management and policy
Even before medical school, Royan began working on the project that would become her capstone. She studied dust generated from building demolitions in Detroit and used the data to advise the city, in real time, on safe and cost-effective demolition. Working with the EPA and the State of Michigan, Royan composed best practices for demolition in Detroit that are now in place.
"As a doctor, Regina will always be thinking about what affects health beside health care," says Goold. "Her project in Detroit is a case of one's ZIP code being seen as more important than their genetic code. Regina really gets that."
Like most Path of Excellence students, Royan wants to continue her pursuits into residency and beyond. "I met and learned from physicians who were using health policy work as a complement to their careers in academic medicine," she says. "Their mentorship was invaluable as I decided how I want to shape my future."

MEDICAL HUMANITIES
SARAH BANKS (third-year medical student): "Exploring Ancient Medicine," a series of seminars. Banks is pictured here outside a glass-encased child mummy at the U-M Kelsey Museum of Archaeology
PATH DIRECTOR: Mary Blazek, M.D., MEHP, associate professor of psychiatry
Banks' capstone is one example of diverse formats that students employ on the Medical Humanities Path, Blazek says. Many students create artistic products (for example, one student plans a series of paintings about the health struggles of her immigrant family). In Banks' case, the ideas that captivated her grew out of her love of literature and history.
A classics major, Banks wanted to find links between modern medicine and ancient Greece. As she was planning her capstone, U-M's Kelsey Museum of Archaeology was planning an exhibit, The Art and Science of Healing: From Antiquity to the Renaissance. Blazek introduced Banks to the exhibit's curator, Pablo Alvarez, M.Sc., Ph.D., outreach librarian and curator of the U-M Special Collections Library.
"Collaboration with Kelsey was an excellent opportunity to meet with people on campus not involved in the medical school," Banks says, "and to connect the medical and museum communities."
Banks worked with Catherine Person, Kelsey's educational and academic outreach coordinator, on a series of seminars addressing ancient medicine topics in which students had expressed interest, such as medicine and religion in the ancient world and the history of surgery. Laura Hirshbein (M.D. 1997), Ph.D., a clinical professor of psychiatry and an adviser to the humanities path, helped Banks design the seminars to be relevant to medical education. The first seminar, an introduction to the art and science of healing in ancient times, was given by Alvarez in March 2017. Thirty students and eight faculty members attended. The majority rated the seminar "excellent," and many students said that the seminar helped them see medicine as an evolving entity, always changing. A second seminar is now in development.
Learn more about Paths of Excellence. For information about supporting the program, contact John Copeland.