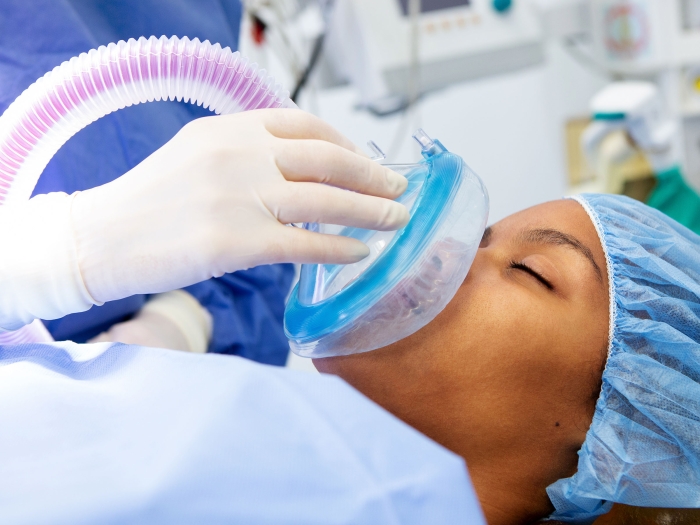
It begins with shortness of breath. And for approximately one-third of patients, acute respiratory distress syndrome (ARDS) ends in death. For those who survive, their lives are often turned upside-down. Michigan Medicine researchers have been investigating the downstream effects of ARDS for years. During the COVID-19 pandemic, their work has relevance for hundreds of thousands of new patients.
"Only a third or fewer of COVID-19 patients who develop respiratory failure die," says Theodore (Jack) Iwashyna, M.D., Ph.D., professor of critical care medicine. "Most survive, and we need research that helps them not just survive but really heal."
A team led by Iwashyna wanted to look more closely at how being hospitalized for ARDS affected people months after they were discharged. The researchers interviewed dozens of patients from around the nation. "As we knew from past research, people had new disabilities ranging from general fatigue and weakness to where they couldn't remember things," says Katrina Hauschildt, a U-M sociology graduate student and first author on the study. "A lot of people had emotional difficulties coming to terms with just how sick they had been — a kind of PTSD from being in the ICU."
The team found that many respiratory failure patients experience what is known as financial toxicity, defined as the financial burdens and related distress of medical care. The team also reported emotional distress related to insurance issues and unpaid bills, reduced physical well-being because of the inability to receive follow-up care due to cost, an increased reliance on family and friends to help cover expenses, and other material hardships. Said one patient: "In the next couple of months, I may end up being homeless because of the financial aspect of it."
While these cases may seem extreme, they were not rare. And many patients described having to make hard choices about whether they could afford rehabilitation — and stopping early when their coverage ran out, even though they were not yet recovered.
A 61-year-old woman described not having the equipment when she tried to go home: "I could pick one item that I wanted," of the hospital bed, wheelchair, and walker she needed, "because the insurance would only pay for one item."
Hauschildt says physicians and other health care providers can help patients access financial resources, but the resources available are really up to policy makers. For example, the study found that patients who were already on public insurance before their illness reported less of an out-of-pocket financial impact. "Communities that put a safety net in place for ARDS and COVID-19 survivors will ultimately have better healing and recovery."
This work was supported by the National Institutes of Health, National Heart, Lung and Blood Institute as part of the Prevention and Early Treatment of Acute Lung Injury (PETAL) Network.
A version of this article was originally published on the U-M Health Lab Blog.